

CARF Accreditation
The Gold Standard Of Excellence
 CARF accreditation is the highest level of accreditation possible for rehabilitation programs.
The following programs at Johnson Rehabilitation Institute at Ocean University Medical Center are accredited by CARF:
CARF accreditation is the highest level of accreditation possible for rehabilitation programs.
The following programs at Johnson Rehabilitation Institute at Ocean University Medical Center are accredited by CARF:
- General Inpatient Rehabilitation
- Inpatient Stroke Rehabilitation
- Inpatient Brain Injury Rehabilitation
What our CARF accreditation means to you
CARF® International is an independent, nonprofit organization that surveys and accredits more than 59,000 programs worldwide. CARF accreditation means that CARF surveyors have rigorously examined our services and operations to independently verify that each program strictly adheres to CARF’s internationally recognized standards of patient care and quality.
Our accreditation is also evidence of our commitment to:
- Involve you and your family with planning your care;
- Provide you with treatment and services that will help you achieve the best outcomes possible;
- Respect your cultural preferences;
- Address public health and safety concerns, such as creating a culture of safety and emergency preparedness;
- Maintain efficient, cost-effective management practices that are based on patient outcomes and satisfaction;
- Remain accountable to our funding sources, referral agencies and the community at large.
For more information about CARF International, the standards, or the accreditation process, visit their website.
Answers to Frequently Asked Questions about Our Accredited Programs
Brain Injury Program FAQs
Johnson Rehabilitation Institute at Ocean University Medical Center, is a 40 bed inpatient rehabilitation hospital attached to an acute care hospital. It is the only acute comprehensive inpatient rehabilitation facility in Ocean County that is accredited by CARF* with a Stroke and Brain Injury Specialty Program and an Outpatient Medical Services Speciality Program.
- Our Mission: To deliver goal-oriented and comprehensive inpatient rehabilitation by creating individualized programs that address each person served’s physical, communicative, cognitive, and psychosocial needs.
- Our Vision: To empower every person served to achieve their highest level of independence, rebuild their self-confidence, and return to a meaningful and fulfilling life within their community.
*The Commission on Accreditation of Rehabilitation Facilities (CARF) is a national, not-for-profit organization whose sole concern is to promote quality services for people with disabilities.
Johnson Rehabilitation Institute at Ocean University Medical Center provides a comprehensive, interdisciplinary and functionally-based treatment program that helps our patients recover and return to their optimal level of function.
The inpatient Brain Injury Speciality Acute Rehabilitation program is provided 365 days per year led by our physiatrist who directs the clinical team to provide 24-hour nursing services, 24-hour physician medical oversight and therapy services tailored to your needs. Therapy is available seven days a week between the hours of 8 AM and 4:30 PM to meet the needs of the individualized therapy programs. Case Management is available Monday through Friday between the hours of 8 AM and 5:30 PM and by appointment on weekends
The treatment program directly provides medical, nursing, case management, dietary, physical therapy, occupational therapy, speech therapy, recreation therapy and a prosthetist/orthotist as needed.
Other services available on site through Ocean University Medical Center to all patients every day based on individual patient needs include:
- Medical consultations
- Diagnostic radiology services
- Laboratory services
- Pharmacy services
- Education and Training
The program delivers training and education services via information and communication technologies utilizing cell phone technology to the geographic areas that include the person served, their families, or their support systems.
The Acute Brain Injury Specialty Program serves inpatients who have sustained a traumatic or non traumatic brain injury. Patients who have an eligible admitting diagnosis may also have ongoing or new comorbid conditions. A candidate for our program must have a medical condition that is stable enough to allow participation in therapies and functional progression. Patients who are on a ventilator, or are in a coma, require telemetry or who are actively receiving chemotherapy infusions are not accepted for admission. Patients with serious psychological disturbances or aggressive behavior are not accepted if they are considered unsafe to themselves or others or unmanageable on a non-psychiatric unit.
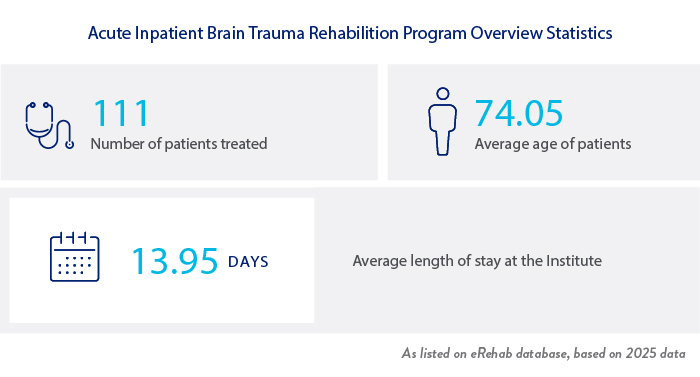
Our Physicians (Physiatrists) are Board Certified in Physical Medicine and Rehabilitation and Brain Injury Medicine. Our clinical team includes therapists who are Certified Brain Injury Specialists, (CBIS), Certified Stroke Rehabilitation Specialists, (CSRS), Geriatric Clinical Specialists, and have training in specific neurological techniques (NDT, PNF, Neuro-IFRAH) as well as crisis prevention training from the Crisis Prevention Institute, (CPI). Many of our nurses are Certified Rehabilitation Registered Nurses (CRRN).
Johnson Rehabilitation Institute at Ocean University Medical Center provides individualized multidisciplinary treatment in a spacious therapeutic environment using advanced technology including: Zero G, Vital Stim Plus, Visi Pitch, Raphael Smart Glove and Virtual Reality System.
Our facility includes accessible rooms and a nursing unit equipped with a wander alter system. Our state-of-the-art gym provides a healing environment to maximize the rehabilitation process and promote family interaction.
Johnson Rehabilitation Institute at Ocean University Medical Center’s patients are scheduled for a minimum of 3 hours of therapy per day for 5 days. However, if medically necessary, a modified program may be scheduled for 15 hours of therapy over the course of 7 days.
In addition to the physical, occupational and speech therapy services provided, you may also participate in recreational therapy and time with an orthotist or prosthetist if indicated in your individual plan of care.
The clinical team, in consultation with the patient/family, determines the estimated time for your inpatient recovery based on clinical needs. Once this duration is finalized the case manager or the physician will communicate this to you.

Patients are typically referred from hospital and physician providers throughout the Hackensack Meridian Health Network or local, regional, statewide, and national facilities. Patients may also be referred from home or subacute settings. To be eligible for inpatient rehabilitation, individuals must demonstrate medical stability, a willingness and ability to tolerate and benefit from at least three hours of therapy a day and have a need for the unique expertise of a rehabilitation physician 24 hours a day.
We accept insurance payments from government-sponsored (Medicare and Medicaid) and third-party payers, including commercial insurances, workers’ compensation, motor vehicle insurance and private/self-pay. All insurances are verified for coverage prior to the initiation of services. Fees for services can be obtained through the Client Services department.
Your treatment team will work with you to optimize your functional outcomes and meet your goals to reentry into your home and community. All patients are evaluated to see how much help they need to do functional activities on admission, and again prior to discharge. Both mobility skills (such as walking and moving from lying down to sitting up) and self care skills (getting dressed and bathing) are measured. Each person’s goals and activities are unique and will require different levels of support or equipment. Therefore, prior to you leaving the Institute, your team will work with you and your family to feel comfortable and confident with your transition.
Patients at our institution achieved the following outcomes:
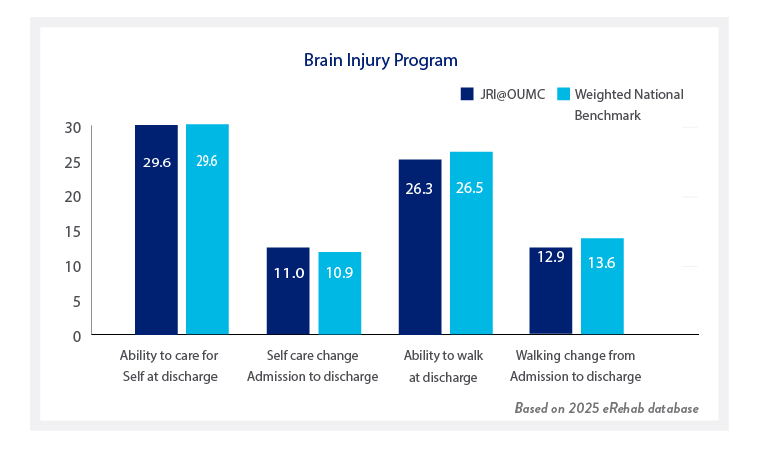
Our goal is to return every patient back to his or her own home whenever possible. Most patients continue receiving follow-up therapy services after they’re discharged home.
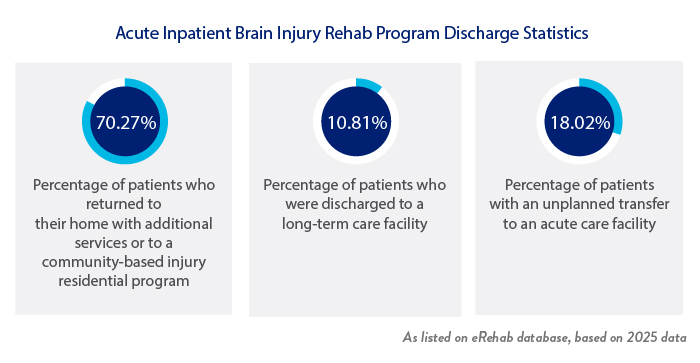
When a patient is discharged from the Institute, they receive a follow-up mailed survey approximately 90 days after they leave. The patient is asked to rate their level of satisfaction in five different areas.
Likely to Recommend the Facility - Very Good or Excellent - 100%

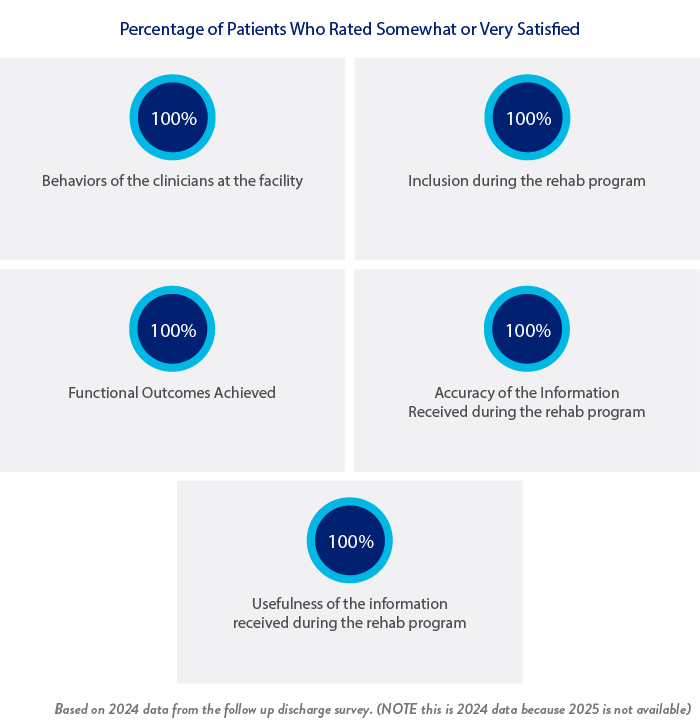
General Inpatient Rehabilitation FAQs
Johnson Rehabilitation Institute at Ocean University Medical Center, is a 40 bed inpatient rehabilitation hospital attached to an acute care hospital. It is the only acute comprehensive inpatient rehabilitation facility in Ocean County that is accredited by CARF* with a Stroke and Brain Injury Specialty Program and an Outpatient Medical Services Speciality Program.
- Our Mission: To deliver goal-oriented and comprehensive inpatient rehabilitation by creating individualized programs that address each person served’s physical, communicative, cognitive, and psychosocial needs.
- Our Vision: To empower every person served to achieve their highest level of independence, rebuild their self-confidence, and return to a meaningful and fulfilling life within their community.
*The Commission on Accreditation of Rehabilitation Facilities (CARF) is a national, not-for-profit organization whose sole concern is to promote quality services for people with disabilities.
Johnson Rehabilitation Institute at Ocean University Medical Center provides a comprehensive, interdisciplinary and functionally-based treatment program that helps our patients recover and return to their optimal level of function.
The acute inpatient rehabilitation program is provided 365 days per year led by our physiatrist who directs the clinical team to provide 24-hour nursing services, 24-hour physician medical oversight and therapy services tailored to your needs. Therapy is available seven days a week between the hours of 8 AM and 4:30 PM to meet the needs of the individualized therapy programs. Case Management is available Monday through Friday between the hours of 8 AM and 5:30 PM and by appointment on weekends
Your treatment program consists of physical therapy, occupational therapy, speech therapy, recreation therapy and a prosthetist/orthotist as needed.
Other services available on site through Ocean University Medical Center to all patients every day based on individual patient needs include:
- Medical consultations
- Diagnostic radiology services
- Laboratory services
- Pharmacy services
- Education and Training
The program delivers training and education services via information and communication technologies utilizing cell phone technology to the geographic areas that include the person served, their families, or their support systems.
Adult patients with the following rehabilitation diagnoses are admitted for treatment:
- Stroke
- Brain injury
- Spinal cord injury
- Amputations
- Neurological conditions
- Orthopedic conditions
- Cardiac conditions
- Other general medical/surgical conditions
A candidate for our program must have a medical condition that is stable enough to allow participation in therapies and functional progression.
JRI@OUMC serves patients who have traumatic and non-traumatic incomplete spinal cord injuries of all levels (ranging C1-S5, ASIA Impairment Scales B, C, D, and E), but not complete spinal cord injuries (i.e. ASIA Impairment Scale A)
Patients who are on a ventilator or who are in a coma, require telemetry or who are actively receiving chemotherapy infusions are not accepted for admission. Patients with serious psychologic disturbances or aggressive behavior are not accepted if they are considered unsafe to themselves or others or unmanageable in a non-psychiatric unit.

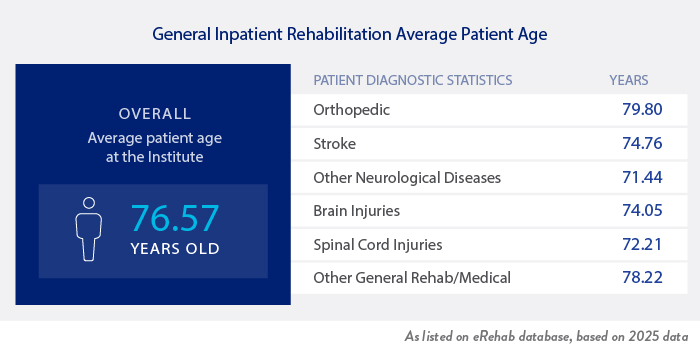
Johnson Rehabilitation Institute at Ocean University Medical Center’s patients are scheduled for a minimum of 3 hours of therapy per day for 5 days. However, if medically necessary, a modified program may be scheduled for 15 hours of therapy over the course of 7 days.
In addition to the physical, occupational and speech therapy services provided, you may also participate in recreational therapy and time with an orthotist or prosthetist if indicated in your individual plan of care.
The clinical team, in consultation with the patient/family, determines the estimated time for your inpatient recovery based on clinical needs. Once this duration is finalized the case manager or the physician will communicate this to you.
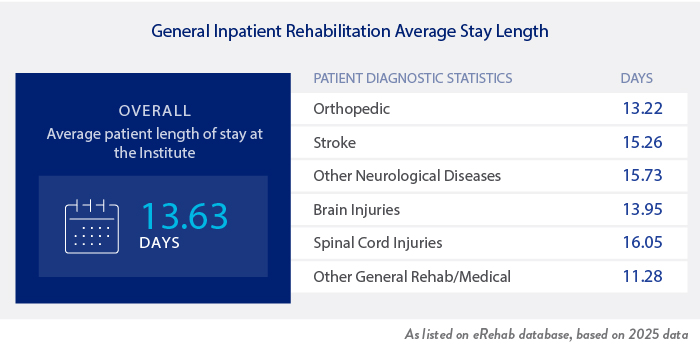
Johnson Rehabilitation Institute at Ocean University Medical Center is attached to an acute care hospital that provides emergency care, neurology, pulmonology, cardiology and other services.
We work with Ocean University Medical Center to ensure the following services are available to our patients including but not limited to: pharmacy, laboratory, diagnostic imaging, dietitian/nutritional support, spiritual services, respiratory therapy, specialized wound care and other services as needed per the patient's plan of care. Services are provided based on hours of service provided at the acute care side of the hospital and meet regulatory required timeframes.
Patients are typically referred from hospital and physician providers throughout the Hackensack Meridian Health Network or local, regional, statewide, and national facilities. Patients may also be referred from home or subacute settings. To be eligible for inpatient rehabilitation, individuals must demonstrate medical stability, a willingness and ability to tolerate and benefit from at least three hours of therapy a day and have a need for the unique expertise of a rehabilitation physician 24 hours a day.
We accept insurance payments from government-sponsored (Medicare and Medicaid) and third-party payers, including commercial insurances, workers’ compensation, motor vehicle insurance and private/self-pay. All insurances are verified for coverage prior to the initiation of services. Fees for services can be obtained through the Client Services department.
Your treatment team will work with you to optimize your functional outcomes and meet your goals to reentry into your home and community. All patients are evaluated to see how much help they need to do functional activities on admission, and again prior to discharge. Both mobility skills (such as walking and moving from lying down to sitting up) and self care skills (getting dressed and bathing) are measured. Each person’s goals and activities are unique and will require different levels of support or equipment. Therefore, prior to you leaving the Institute, your team will work with you and your family to feel comfortable and confident with your transition. Patients at our institution achieved the following outcomes:
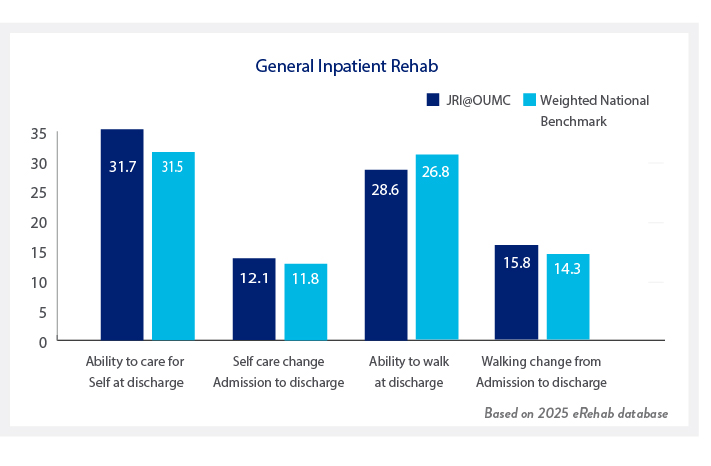
It is our goal to return every patient back to his/her own home, whenever possible. Most patients continue to receive follow up therapy services after they are discharged home. Percentage of patients who returned to their home:
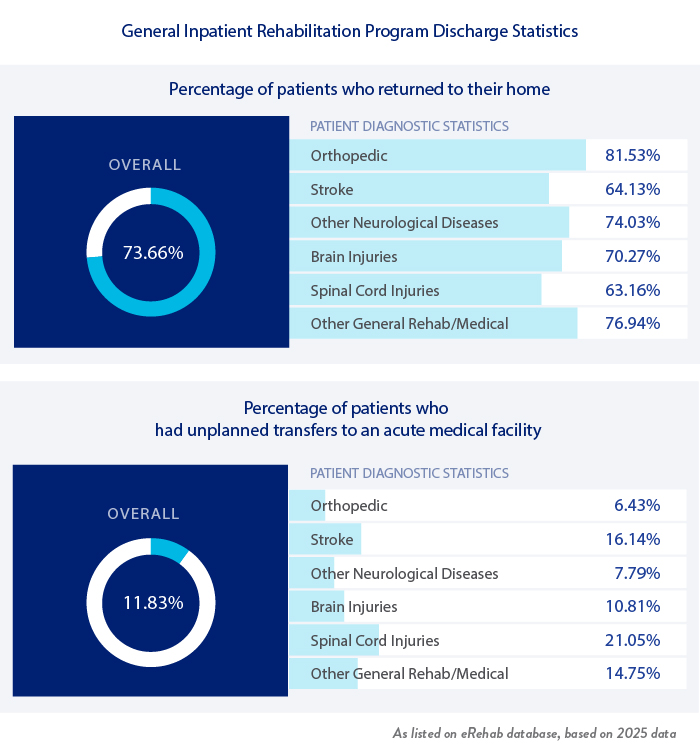
When a patient is discharged from the Institute, they receive a Patient Satisfaction Questionnaire. Patients answer the questions on a scale of 1-10 rating their satisfaction with program services in many areas.
NPS Likely to Recommend Facility : 83.9% vs 74.0% benchmark
Based on 2025 NRC Health Data

Johnson Rehabilitation Institute at Ocean University Medical Center places a priority on preventing any type of harm to our patients. Pressure ulcers can be painful and cause other complications, like a reduction in mobility and infections. Johnson Rehabilitation Institute at Ocean University can help prevent and treat pressure ulcers by understanding which patients are at higher risk, ensuring frequent changes in the patient's position, providing proper nutrition, and using specialized beds to reduce pressure on the skin. According to Medicare.gov, Johnson Rehabilitation Institute at Ocean University Medical Center performed better than the national average in preventing or improving skin injury.
Fall-related injuries are a leading cause of morbidity and mortality among inpatient rehabilitation patients, and are an important health outcome to monitor. Falls with major injury can cause new physical limitations, disability, and depression. Johnson Rehabilitation Institute at Ocean University Medical Center prevents or reduces falls by providing appropriate patient care and sufficient support. According to Medicare.gov, Johnson Rehabilitation Institute at Ocean University Medical Center performed better than the national average in preventing falls with major injury.
Johnson Rehabilitation Institute at Ocean University Medical Center continues to be a proud recipient of Ocean University Medical Center Foundation grants. The institute has received funding for technology items, staff advance training and community outreach projects.
Inpatient Stroke Rehabilitation FAQs
The Stroke Specialty Program serves inpatients who have sustained an ischemic or hemorrhagic stroke. Patients who have an eligible admitting diagnosis may also have ongoing or new comorbid conditions. A candidate for our program must have a medical condition that is stable enough to allow participation in therapies and functional progression.
Patients who are on a ventilator, or in a coma, require telemetry or who are actively receiving chemotherapy infusions are not accepted for admission. Patients with serious psychologic disturbances or aggressive behavior are not accepted if they are considered unsafe to themselves or others or unmanageable in a non-psychiatric unit.
Johnson Rehabilitation Institute at Ocean University Medical Center provides a comprehensive, interdisciplinary and functionally-based treatment stroke program that helps our patients recover and return to their optimal level of function.
The acute inpatient stroke rehabilitation program is provided 365 days per year led by our physiatrist who directs the clinical team to provide 24-hour nursing services, 24-hour physician medical oversight and therapy services tailored to your needs. Therapy is available seven days a week between the hours of 8 AM and 4:30 PM to meet the needs of the individualized therapy programs. Case Management is available Monday through Friday between the hours of 8 AM and 5:30 PM and by appointment on weekends. Your treatment program consists of physical therapy, occupational therapy, speech therapy, recreation therapy and a prosthetist/orthotist as needed.
Other services available on-site through Ocean University Medical Center to stroke patients every day based on individual patient needs include:
- Medical consultations
- Diagnostic radiology services
- Laboratory services
- Pharmacy services
- Education and training
- Risk management: Risk factors for stroke are identified and a plan to manage these controllable factors is implemented. These include diabetes, atrial fibrillation, hypertension and/or hyperlipidemia.
- Safety assessment, education and implementation: Safety for stroke patients includes individual adaptive safety measures and direct referrals to local community services upon discharge.
- Therapy: Focuses on addressing areas of limitation such as dysphagia (swallowing disorder), mobility, self care, speech/language, cognition, behavior and/or assistive technology. Considerations for post-discharge needs include smoking cessation, durable equipment needs, driver training, environmental/home modifications, leisure and recreation interests, occupation, orthoses and access to emergency care.
The program delivers training and education services via information and communication technologies utilizing cell phone technology to the geographic areas that include the person served, their families, or their support systems.
Johnson Rehabilitation Institute at Ocean University Medical Center’s patients are scheduled for a minimum of 3 hours of therapy per day for 5 days. However, if medically necessary, a modified program may be scheduled for 15 hours of therapy over the course of 7 days.
In addition to the physical, occupational and speech therapy services provided, you may also participate in recreational therapy and time with an orthotist if indicated in your individual plan of care.
Patients are typically referred from hospital and physician providers throughout the Hackensack Meridian Health Network or local, regional, statewide, and national facilities. Patients may also be referred from home or subacute settings. To be eligible for inpatient rehabilitation, individuals must demonstrate medical stability, a willingness and ability to tolerate and benefit from at least three hours of therapy a day and have a need for the unique expertise of a rehabilitation physician 24 hours a day.

The clinical team, in consultation with the patient/family, determines the estimated time for your inpatient recovery based on clinical needs. Once this duration is finalized the case manager or the physician will communicate this to you.
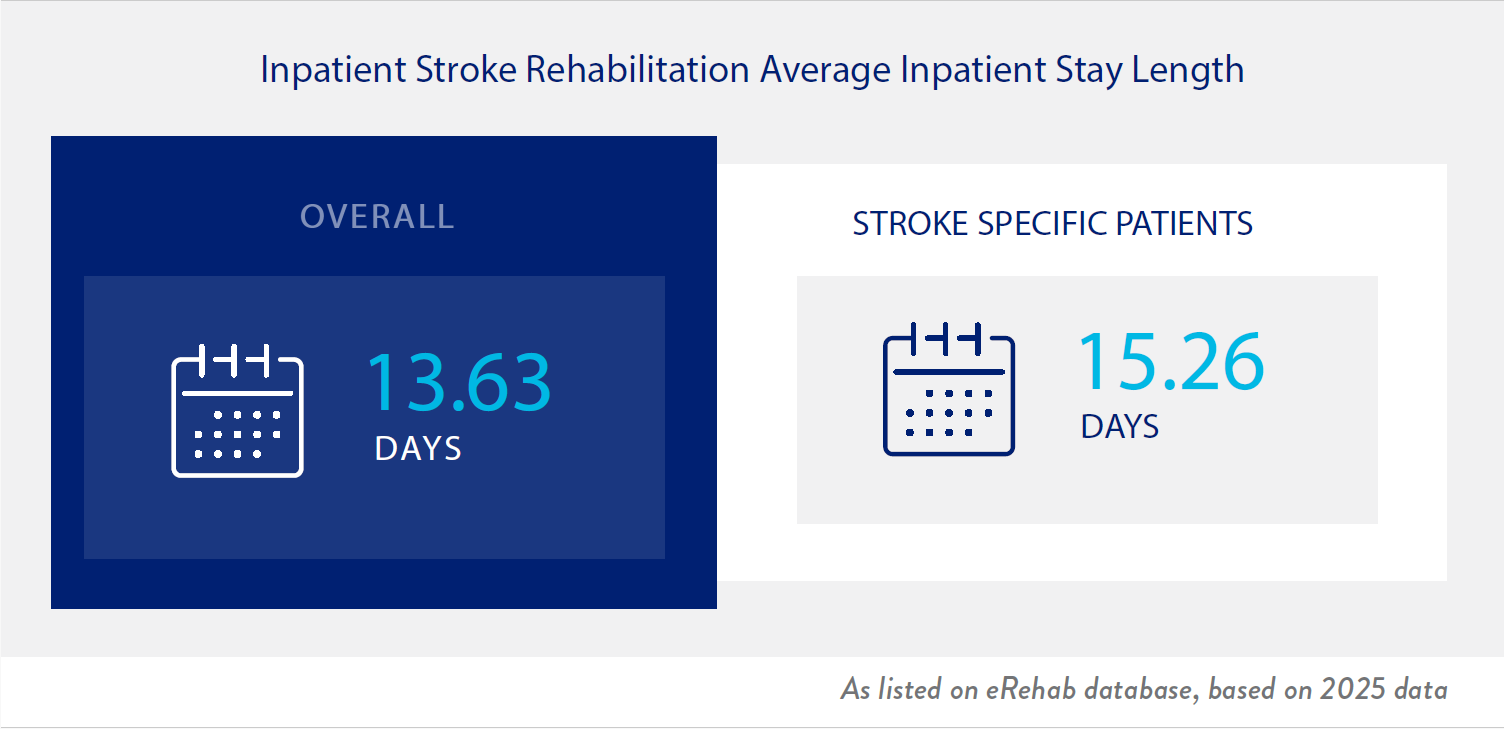
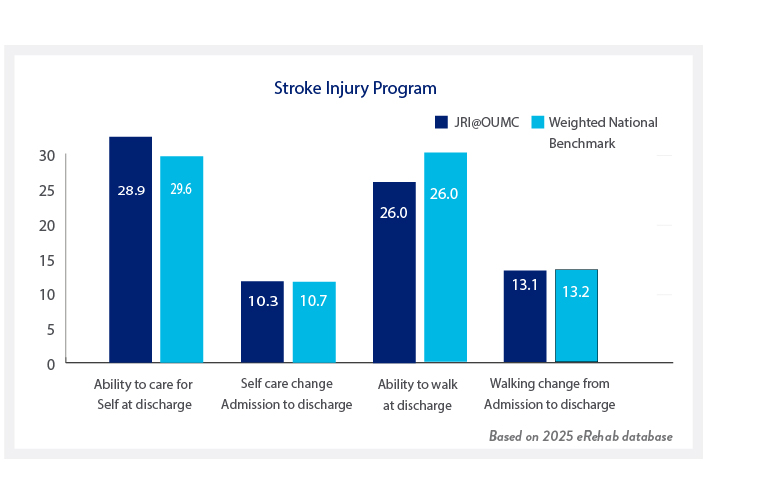
Your treatment team will work with you to optimize your functional outcomes and meet your goals to reentry into your home and community. All patients are evaluated to see how much help they need to do functional activities on admission, and again prior to discharge. Both mobility skills (such as walking and moving from lying down to sitting up) and self care skills (getting dressed and bathing) are measured. Each person’s goals and activities are unique and will require different levels of support or equipment. Therefore, prior to you leaving the Institute, your team will work with you and your family to feel comfortable and confident with your transition. Patients at our institution achieved the following outcomes:
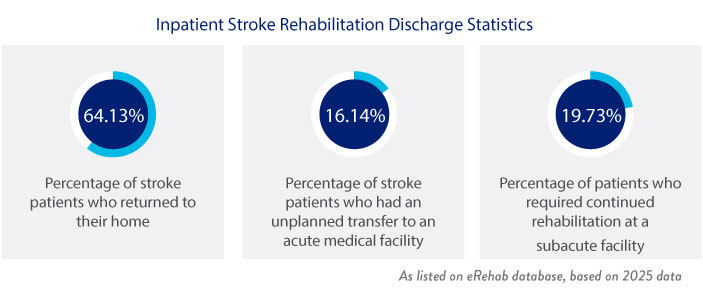
Our goal is to return patients back to their own homes whenever possible. Most patients continue to receive follow up therapy services after they are discharged home.
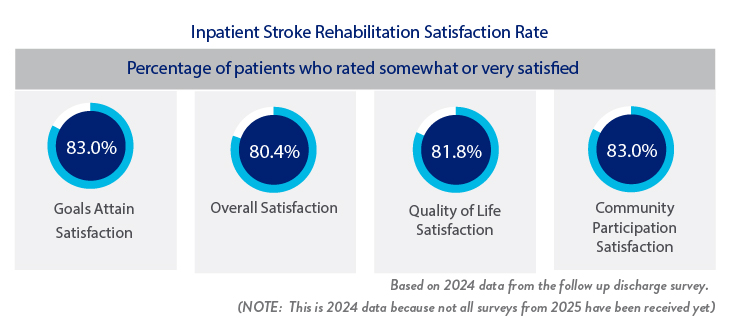
When a patient is discharged from the Institute, they receive a follow-up mailed survey approximately 90 days after they leave. The patient is asked to rate their level of satisfaction in five different areas.
Likely to Recommend the Facility - Very Good or Excellent - 81%

After 90 days from discharge from JRI @OUMC, 80.65% of our patients reported the ability to perform self care activities (bathing, dressing, grooming, eating) was better than at the time of discharge, and 77.42% reported that the ability to move around at home was better than at the time of discharge.
Based on 2025 data from the follow up discharge survey.